Millions of Americans could face dramatically higher health insurance bills next year as enhanced Affordable Care Act (ACA) premium tax credits are set to run out.
Why It Matters
The enhanced subsidies, which lower monthly premiums for people across income levels, expire at the end of the year, raising the prospect of substantial increases for enrollees, unless Congress intervenes.
The ACA marketplace, established in 2010, offers health insurance to people who don’t qualify for Medicaid and aren’t covered through an employer. In 2020, Congress introduced the Enhanced Premium Tax Credit to help lower costs during the COVID-19 pandemic. The expanded subsidies significantly reduced monthly premiums—and for some low-income enrollees, brought them down to $0.
According to the Congressional Budget Office, letting the subsidies lapse would cause next year’s premiums to more than double for many enrollees and leave an estimated 2 million additional people uninsured.
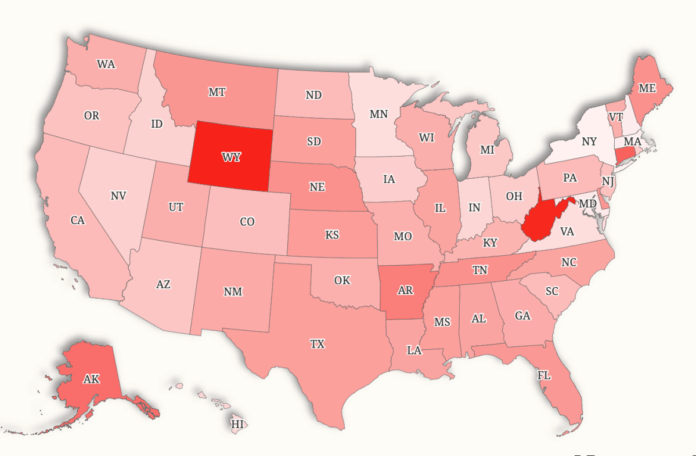
States Facing Highest Increases
According to analysis by KFF Health, the financial shock will be sharpest for older adults at middle incomes—particularly those just above the previous eligibility cutoff for ACA subsidies. Among all income tiers examined, the current enhanced credits yield the biggest benefit for those at 401 percent of the federal poverty level, which is equal to $62,757 for an individual in the contiguous U.S. (with higher thresholds in Alaska and Hawaii).
For a 60-year-old at that income level, the expiration of enhanced credits would at least double average annual premiums for a benchmark silver plan in 46 states and Washington, D.C. In 19 of those states, premiums would at least triple, consuming more than a quarter of a person’s yearly income.
The steepest increases occur in:
Wyoming: +$22,452 per year
West Virginia: +$22,006
Alaska: +$19,636
On why premiums will rise the most in these states, Professor Stacey B. Lee, professor at Johns Hopkins University and CEO of Praxis Pacisci, a negotiations training institute, told Newsweek: